Experts want more data before making the jabs more widespread.
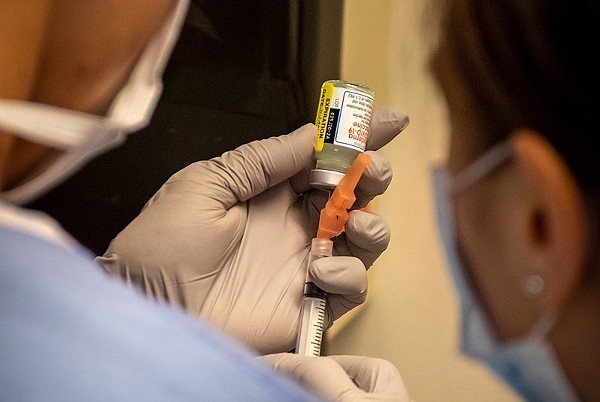
In the United States, booster shots of Pfizer and BioNTech’s COVID-19 vaccine won’t be widely available to the general public starting this week. Instead, only certain groups will have access to a third dose of the vaccine: people 65 years and older, individuals 18 and older who are at high risk of severe COVID-19, and those whose jobs put them at high risk of getting infected.
These new guidelines come after nearly a week of intense debate and last-minute seesawing over who should be eligible for an extra dose.
The U.S. Food and Drug Administration on September 22 granted an emergency use authorization that opened the door for boosters for these individuals, following the unanimous recommendation on September 17 by its panel of expert advisers.
But on September 23, an advisory panel for the U.S. Centers for Disease Control and Prevention rejected boosters for those who might be exposed to the coronavirus on the job. Panelists argued that the vaccine still works extremely well and there’s no evidence of waning protection against hospitalization in this group. Still, the panel did vote that the older age group and individuals 50 to 64 years old who have health conditions, such as heart disease, diabetes or obesity, that put them at high risk of severe disease should get a booster dose.
For those ages 18 to 64 with underlying conditions, their individual risk and benefit should factor into booster decisions, the CDC panel said.
Hours later, CDC director Rochelle Walensky tweaked the guidelines to once again include people whose jobs put them at risk of being exposed to SARS-CoV-2, the virus that causes COVID-19. That group includes essential workers like health care professionals, people who live in group settings such as homeless shelters and anyone whose job brings them within six feet of others. Like with younger people with underlying conditions, individual risk and benefit should be weighed. “In a pandemic, even with uncertainty, we must take actions that we anticipate will do the greatest good,” Walensky said in a Sept. 24 statement.
The guidance applies only to people who received the Pfizer vaccine. Decisions on boosters for Moderna’s and Johnson & Johnson’s jabs — the other two COVID-19 vaccines available in the United States — still lie ahead.
Getting unvaccinated people vaccinated will still have the biggest impact on the pandemic, as well as following other public health measures like wearing masks, Katherine Poehling, a pediatrician at Wake Forest School of Medicine in Winston-Salem, N.C., said at the Sept. 23 CDC meeting. Two doses of the Pfizer vaccine are still highly effective for most people, she noted, even as some groups become eligible for a booster shot.
Both agencies’ actions are more limited in scope than what the Biden administration proposed in August. Officials had announced plans to offer a third dose of Pfizer’s vaccine to the general public at least six months after vaccination starting September 20, pending an OK from the FDA.
Since officials unveiled that plan, it’s been widely debated. Some researchers — including Pfizer scientists — argue that because the vaccine’s protection against infections is waning, that could foreshadow a possible dip in protection against severe disease too. So the time to bolster everyone’s protection with a third dose is now, these researchers say. But others disagree, contending that it’s more important to focus on getting doses to unvaccinated people first, and that many younger, healthy vaccinated people remain well-protected against severe disease and death after just two doses.
Third doses are already authorized for moderately to severely immunocompromised people who may not develop good protection from the initial shots. The case for another dose was obvious for that group, says Mark Slifka, a viral immunologist at Oregon Health & Science University in Portland who wasn’t involved with the FDA panel. The data were “clear as day that the third dose was important” and could help boost the levels of protective antibodies in some patients.
But moving forward for the general population requires more specialized consideration, Slifka notes. “I think part of it comes down to what’s our level of risk tolerance.”
Here are some of the key questions that influenced the FDA panel’s recommendation.
Is vaccine effectiveness starting to wane?
COVID-19 vaccines are still largely keeping people out of the hospital in the United States, studies show (SN: 8/31/21). Even as infections among vaccinated people go up, protection against hospitalization and death remains high, CDC epidemiologist Sara Oliver said at the September 17 meeting.
That’s true for all three vaccines — developed by Pfizer, Moderna and J&J — available in the United States even with the spread of the highly contagious delta variant. Before delta dominated in the country, estimates of vaccine effectiveness against hospitalization in adults 18 and older ranged from 84 to 97 percent. That’s compared with 75 to 95 percent effectiveness after the variant took over, Oliver said. Effectiveness against infection, on the other hand, has dipped from 72 to 97 percent before delta to around 40 to 84 percent.
Still, data from Israel — the first country to vaccinate the majority of its population against COVID-19 — hint that over time Pfizer’s COVID-19 vaccine becomes less effective at preventing severe disease, particularly in people age 60 and older. That trend spurred public health officials there to begin offering a booster dose to that age group July 30 amid a spike in cases.
That third dose seems to have helped. People age 60 and older who didn’t receive a booster were 11 times as likely to be infected with the coronavirus and nearly 20 times as likely to develop severe disease compared with those who got a third dose at least 12 days earlier, researchers reported September 15 in the New England Journal of Medicine. Preliminary data presented at the September 17 meeting suggest that the same trend may occur in people ages 40 to 59.
The booster brings vaccine efficacy back up to levels seen before delta came on the scene, Sharon Alroy-Preis, head of public health services at Israel’s Ministry of Health, told the FDA panel. “It’s like a fresh vaccine.”
It’s less clear, however, that protection against the worst of COVID-19 wanes in younger people, too, contributing to the FDA panel’s recommendation for boosters for those age 65 and older. But that should become clearer in the coming months, as researchers continue to monitor the situation.
In Israel, everyone over age 12 became eligible on August 29 for a third shot at least five months after a second dose. That decision was made because officials wanted to control the latest surge in cases, and limiting transmission would have been difficult without vaccinating everyone eligible, Alroy-Preis said.
Estimates suggest that transmission in Israel is indeed slowing. By one measure, infected people tend to pass the virus on to fewer than one other person, meaning the outbreak could begin to fizzle out. While hospitalizations and severe cases have stabilized since people began receiving boosters, however, the overall number of COVID-19 cases remains high.
That disparity may exist because the country opened schools on September 1 and many Israelis have gathered in holiday celebrations, Alroy-Preis said. But once things settle down, officials will likely have a better sense of where things stand. “We feel the booster effect, but we are not over the fourth wave yet,” she said.




















