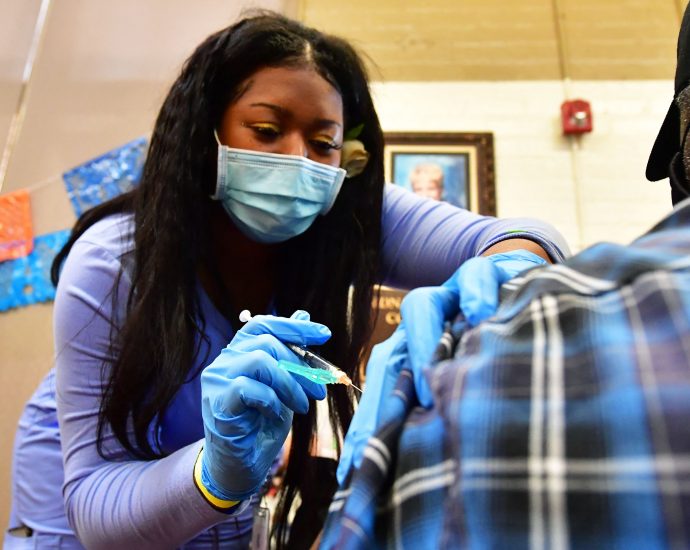
New COVID booster vaccines built for the latest variants are here and should be more effective. But there are still some unknowns

A new generation of COVID booster shots are now available to most people 12 years of age and older in the U.S. The Food and Drug Administration authorized new formulations of the Moderna and Pfizer-BioNTech COVID vaccines for use as a single booster dose just a few weeks ago. That decision was quickly endorsed by an immunization advisory panel at the U.S. Centers for Disease Control and Prevention.
The updated boosters target the newer, widely spread Omicron subvariants of the COVID-causing virus, BA.4 and BA.5, as well as the early 2020 form of the microbe, known as the ancestral strain. On the week ending on September 10, BA.5 was estimated to be responsible for 87.5 percent of news infections in the U.S. This is the first change for the Pfizer and Moderna shots since they were introduced two years ago, when they contained only genetic material from the ancestral form of the virus.
The new booster shots are expected to trigger a better immune response against the new subvariants. Clinical studies of similar two-part COVID boosters, as well as mouse research with these specific formulations, suggest that will be the case. Still, some scientists point out we have no hard evidence the new shots will provide longer-lasting protection than previous boosters. That’s an issue because people are tired of frequent requests to get yet another shot. But the U.S. government is pushing for a rapid and wide rollout before an anticipated increase of cases in fall and winter months.
“It comes at a fortuitous time,” says epidemiologist Ali Khan, dean of the University of Nebraska Medical Center College of Public Health. “As people congregate closer together in winter months, they’re more likely to spread microbes between them. So it’s great timing for what is expected to be a fall wave of cases.”
Here is what we know about the makeup, effectiveness and safety of the new vaccine formulations, which are known as bivalent shots because they contain components of two versions of the virus. We’ll also cover a few things that scientists are still trying to figure out.
WHAT ARE THE UPDATED BOOSTERS MADE OF?
The Pfizer-BioNTech and Moderna COVID vaccines contain snippets of viral genetic material called mRNA. Once injected, it can’t create a whole virus, but it does tell cells to build one isolated piece, the infamous spike protein found on the surface of SARS-CoV-2. When the human immune system detects that protein, it starts to produce antibodies and activate other immune cells that can fight the actual virus.
The updated boosters contain mRNA instructions for both the ancestral spike protein and the one on Omicron BA.4 and BA.5. (The protein from those two subvariants is extremely similar.) This is why the new shots induce a broader immune response. All of the other ingredients—such as lipids, salts and acids, which help protect the mRNA and deliver it to our cells, balance acidity and maintain the stability of the vaccine—haven’t changed from the original formulation. The overall dose of each updated booster is also the same as the original boosters.
“This is part of the benefit of having an mRNA vaccine, where you can change only the variants and keep everything else consistent,” says Gigi Gronvall, a senior scholar at the Johns Hopkins Center for Health Security. “I wish that we had had these updated vaccines earlier.”
HOW EFFECTIVE ARE THE BOOSTERS?
The FDA authorization was based on clinical trials of earlier versions of bivalent boosters (made with components of previous SARS-CoV-2 variants), mouse studies of the current bivalent boosters and real-world experience with the COVID mRNA vaccines. Clinical trials of these newest formulations are still being conducted, so their data did not figure into the go-ahead decision. But many scientists contend that the existing studies provide ample evidence of effectiveness.
In a clinical preprint study evaluating one of Moderna’s earlier bivalent booster versions—which was made with the ancestral form and the original Omicron variant, called BA.1—participants who received the booster had a 7.1-fold rise in neutralizing antibody levels against Omicron. The ones who received the ancestral-only booster had a smaller, 3.8-fold rise in neutralizing antibody levels. An advantage was also seen in neutralizing antibody levels against Omicron BA.4 and BA.5.
A similar result was achieved by an earlier bivalent booster developed by Pfizer and BioNTech. It led to a 9.1-fold rise in neutralizing antibody levels against the original form of Omicron, compared with a 5.8-fold rise obtained by the ancestral-only booster. A smaller advantage was seen in neutralizing antibody levels against BA.4 and BA.5. The mouse studies of the new bivalent boosters showed they also increased neutralizing antibody levels, compared with earlier boosters.
This strategy of using previous clinical data and animal studies is what has been done with influenza vaccines for many years, notes immunologist Alessandro Sette of the La Jolla Institute for Immunology. Flu shots are updated to target newer influenza strains without additional clinical studies. When it comes to the new COVID shots, “obviously, if more data was available, specifically immunogenicity data in humans, that would be better,” Sette says. “But I still think it’s a reasonable path to take.” Like Gronvall, his confidence is buoyed because the overall structure of the updated boosters is very similar to the original ones.
Though Sette is reassured, some other experts believe that the lack of human data about these particular shots could turn into a problem when it comes to building public trust. Epidemiologist Michael Osterholm, director of the Center for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota, says he worries that if people have a concern about the safety or efficacy of the updated boosters, they might not get the shots. “I was hoping we would have immunogenicity data in humans to be able to say that, actually, the immune response is better or at least similar to the current vaccine,” he adds.