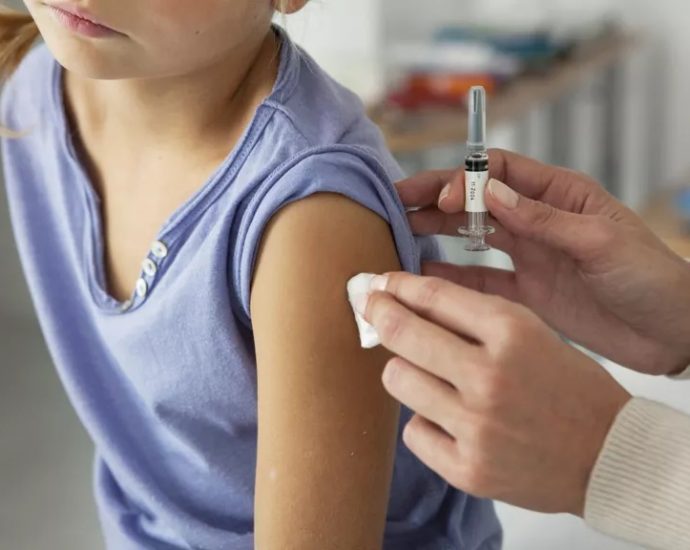
With several coronavirus vaccines barreling through late-stage trials, adults could receive an approved vaccine in months. But even then, we likely won’t know whether any of these vaccines work in children.
Only a handful of coronavirus vaccine trials currently include children as participants — an Oxford-AstraZeneca trial being one of them, Stat News reported. The Chinese company Sinovac Biotech will include children ages 3 to 17 in an upcoming trial, according to ClinicalTrials.gov, but by and large, most vaccine developers have not launched similar trials with participants younger than age 18. And in the U.S., no children have been enrolled in coronavirus vaccine trials, The New York Times reported.
Vaccines typically get tested in adults before children to allow their safety profiles to be fully assessed, and their potential risks minimized, before they’re given to kids. In the case of COVID-19, children generally face a far lower risk of hospitalization and death compared with adults, so taking an untested vaccine could pose higher risks than the virus itself. That said, with data from large adult trials now rolling in, some experts have argued that vaccine trials for kids should start sooner, rather than later.
“The sooner, the better,” said Dr. Flor Munoz-Rivas, an associate professor of pediatric infectious disease at the Baylor College of Medicine in Houston. Given early data gathered in late-stage adult trials, which include thousands of participants, vaccine developers could launch trials for older children ages 12 to 17, she said. If a vaccine appears safe and effective in this group, the trials could then continue in younger and younger children.
In a commentary, published Sep. 18 in the journal Clinical Infectious Diseases, Munoz-Rivas and her colleagues argue that coronavirus vaccine trials for children “should begin now.” To delay such trials could mean delaying “our recovery from COVID-19 and unnecessarily prolong[ing] its impact upon children’s education, health and emotional well-being,” they wrote.
The sooner, the better?
Even though adult hospitalization rates for COVID-19 far outpace those for children, that doesn’t mean kids aren’t being adversely impacted by the disease. The child hospitalization rates for COVID-19 are comparable to those for diseases like chickenpox, Hepatitis A and rotavirus, before vaccines for those infections became widely utilized, the commentary notes.
In addition, about one-third of kids who are hospitalized with COVID-19 end up in intensive care, the authors add. And some infected children develop a condition known as multisystem inflammatory syndrome in children (MIS-C), in which severe inflammation throughout the body causes skin rashes, high fever and abdominal pain, among other symptoms, Live Science previously reported. In a recent study of MIS-C associated with COVID-19, published in The New England Journal of Medicine, 80% of affected children were admitted to the ICU.
As of early September, more than 100 children had died from COVID-19 in the U.S., the authors noted. That’s compared with 188 children who died during the 2019-2020 flu season, according to the Centers for Disease Control and Prevention. “Right now, [both diseases] seem to be similar in terms of mortality, but of course, flu is around for a limited period of time, while COVID circulation is ongoing and we don’t know how long it will last,” Munoz-Rivas said. “The potential for surpassing flu is there, in my opinion.”
An approved vaccine would not only guard children against potential disease and death, but also reduce the spread of COVID-19 from children to others and allow schools to safely resume with fewer distancing measures in place, Dr. Steven Joffe, a bioethics and pediatrics professor at the University of Pennsylvania Perelman School of Medicine, wrote in a commentary in The Washington Post.
“They can definitely transmit the infection, especially older children,” Munoz-Rivas noted.
It’s still unclear how often children below age 10 catch and spread COVID-19, but in a Morbidity and Mortality Weekly Report, published Sep. 28, researchers describe how older teens may be as likely as adults to transmit the virus. Without an approved vaccine for those under age 18, the effort to curb viral spread from children will remain dependent on other countermeasures, like social distancing and mask wearing, Joffe wrote.
Trials for children
Once trials for children get off the ground, enrolling participants may take longer than it would for adult vaccines, Munoz-Rivas noted. COVID-19 vaccine trials for adults have enrolled thousands to tens of thousands of participants in a matter of months, but “the pace of doing a pediatric study is not usually that fast,” she said. For a child to participate in a trial, their legal guardian must give consent on their behalf, and children ages 7 and older must themselves also agree to participate after receiving a thorough explanation of the study’s requirements and risks, she said.
Even with this involved enrollment process, during the 2009 H1N1 pandemic, “we did very quickly go from adults to children, and down to different age groups,” Munoz-Rivas said. In one trial, “we enrolled hundreds of kids in two weeks.” Initial trials of COVID-19 vaccines in kids would likely enroll a few hundred participants, she said.
Typically, after trials in 12- to 17-year-olds, vaccine developers move on to 5- to 12-year-olds, then to children younger than age 5. “It’s not going to be likely that very young infants will be part of the studies early on,” Munoz-Rivas said.
Just like adult trials, trials with children aim to find the safest and most protective dose for a given vaccine, but data already gathered in adults can hint at what dose might be best. Children in early trials receive smaller doses than adult participants, and if they have no harmful side effects, trial leaders gradually increase this dosage. At the same time, trial leaders monitor the amount of antibodies children produce at each given dose; thanks to their young immune systems, children may not need as high a dose as adults to prompt a strong immune response, Munoz-Rivas said.
That said, this initial immune protection might wear off over time, as studies hint that immunity to seasonal coronaviruses may be short-lived, Live Science previously reported. Immunity to COVID-19, whether gained through natural infection or a vaccine, may similarly wane through time.
So after receiving an initial COVID-19 vaccine, both children and adults may require booster shots sometime in the future, Munoz-Rivas noted. Similarly, older children get boosters for chicken pox and whooping cough after receiving their initial doses in infancy. If possible, both child and adult participants in COVID-19 trials should be monitored after their vaccination, for up to 10 years or so, to determine when and whether a booster is necessary, Munoz-Rivas said. The timing and dosage of these boosters may differ between adults and children, depending on their initial immune responses to the vaccine, she added.
As in adult trials, vaccine developers must be on the lookout for both short- and long-term side effects that emerge in vaccinated children. Mild side effects might include mild fever, muscle aches or soreness at the injection site, as have been noted in adults, while a severe reaction might include severe inflammation or an overblown immune response.
Since vaccines trigger the production of antibodies that target the coronavirus, vaccine developers need to ensure that this immune response is strong enough to be protective, but so strong that it’s harmful to the child.
For instance, while the exact cause of MIS-C is unknown, one recent study found that children with the condition have high concentrations of specific antibodies in their blood; these antibodies grab onto part of the virus called the “receptor binding domain” (RBD), a prime target for vaccines. The new study did not show whether these antibodies actually cause MIS-C — they may only be a sign of the illness — but in a commentary accompanying the report, experts cautioned vaccine developers to watch for any symptoms of MIS-C in vaccinated children. The worry would be that a vaccine could prompt production of specific RBD antibodies and that would somehow drive the onset of MIS-C, but this is highly theoretical and may not prove to be a risk at all, Munoz-Rivas noted.
“The issue is, ‘How well do we understand the mechanism'” of how MIS-C occurs, Munoz-Rivas said. “It’s not necessarily an antibody issue,” and most likely, an effective vaccine would help protect children from MIS-C by protecting them from catching COVID-19 in the first place, she said. Given the direct benefits to children, and indirect benefits to those they interact with, pediatric trials of COVID-19 vaccines should start as soon as possible, she and her co-authors wrote.
“For children, a vaccine has the added benefit of returning them safely to school and extracurricular activities, and allowing them to engage with their world face-to-face once again,” they wrote. “Ensuring acceleration of vaccine clinical trials to warp speed for children will be critical in making this our future reality.”